By Dr. Thomas Schlich, Department of Social Studies of Medicine
Patients’ choices and preferences are shaping surgery much more than commonly thought. Typically, histories of surgical techniques look at scientists and surgeons as the main source of change in surgery. Patients only occur as passive recipients of the developed operations. However, a closer look at how new techniques actually spread provides a different picture.
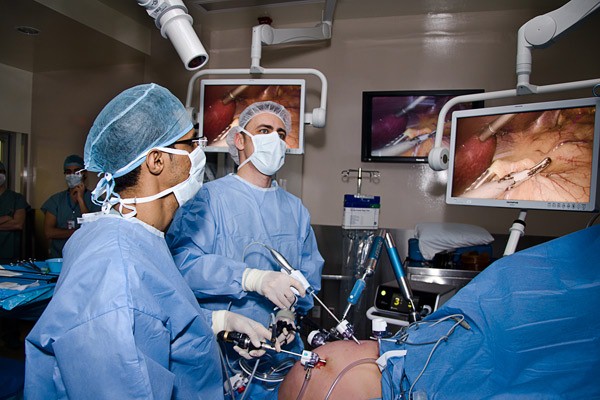
Today, for example, minimally invasive surgery is a wide-spread way of performing a wide variety of operations. With this technique of “keyhole surgery,” surgical interventions are performed through a small incision with the help of a long thin tube with a camera at its end. This tube is passed through the incision along with special instruments which allow the operator to perform the operation within the patient’s body without large incisions. This technique results in much faster recuperation, less pain and less disability than traditional open surgery.
Since the 1990s, gall bladder removal, a common procedure which used to be one of the “bread and butter” operations of general surgery, has been almost completely replaced by its minimally invasive version, laparoscopic cholecystectomy. Surgeons at the time felt that the fast uptake of the new technology was largely driven by patients and many of them found it problematic that patient demand should determine whether the technique was used or not. They emphasized the lack of control of this process by calling it an “explosion” made possible by a “Wild West” mentality.
Surgeons in the academic centers of excellence in particular thought that this over-enthusiasm needed to be reined in and that a solid data base about the benefits and risks needed to be created. As a result, the first Randomized Clinical trial (RCT) on the technique of laparoscopic cholecystectomy was started at McGill University. Other such trials had been attempted before but were never successfully completed – the challenge being that not enough patients were willing to be attributed to the control group which underwent open surgery in order to be able to compare the two methods. They all wanted the new technique!
The McGill group was capable of recruiting enough patients for both groups, which might have been a result of the publicly funded health care system in Canada. However, when the trial was eventually finished (it actually showed the feasibility of laparoscopic cholecystectomy), the technique had already become the standard method of gall bladder removal, again due to its general popularity among patients.
Laparoscopic cholecystectomy is but one example of how patient influence extends even to the methods of scientifically testing new techniques, a trend which is currently being examined by a team of researchers at McGill’s Department of Social Studies of Medicine in their CIHR-funded research project “Disrupting Surgical Practice: The Rise of Minimally Invasive Surgery, 1980-2000” which has resulted in a recently published paper in The Lancet on patient choice, and on the first RCT on laparoscopic cholecystectomy in the Journal of the History of Medicine and Allied Sciences, one of the world’s top medical history journals.
“Patient choice and the history of minimally invasive surgery,” Schlich T. & Tang C., The Lancet, 1 October 2016. doi: http://dx.doi.org/10.1016/S0140-6736(16)31738-X
October 20, 2016
