
A study led by RI-MUHC researcher Nathalie Lamarche-Vane reveals the mechanisms underlying regulation of HER2+ breast cancer progression by the protein CdGAP
Published this month in Cell Reports, a new study by local researchers may lead to better drugs for the treatment of certain aggressive breast cancers. Led by Nathalie Lamarche-Vane, PhD, a senior scientist in the Cancer Research Program at the Research Institute of the McGill University Health Centre (RI-MUHC), the team has discovered a new mechanism by which breast cancer metastasis occurs, at the molecular and cellular level.
“Metastasis occurs when tumour cells detach from the primary tumour and migrate to colonize distant organs, and it is the leading cause of mortality in breast cancer patients,” says Lamarche-Vane, who is also a professor in the Faculty of Medicine and Health Sciences at McGill University. “The mechanisms of metastasis are not well understood, and by learning more about exactly what happens in this process, we can then develop new therapeutics to stop it.”
This study looked at a specific type of breast cancer called HER2+. This subtype represents almost one third of primary breast cancer cases that display early-stage metastasis and poor survival rates when they develop resistance to anti-HER2 therapies. High expression of a protein called CdGAP has been correlated with poor prognosis in this type of cancer, but until this study, it was not known whether CdGAP was required for HER2-driven tumorigenesis and metastasis.
“With this work, we have shown that CdGAP contributes to HER2+ breast tumour development and is central to HER2+ breast cancer metastatic progression,” says Ye Hi, PhD, a research associate in Professor Lamarche-Vane’s laboratory. “At a molecular level, CdGAP is required for TGF-β-induced cell migration and invasion in human HER2+ breast cancer cells, and it interacts with the adaptor protein talin to regulate integrin activation.”
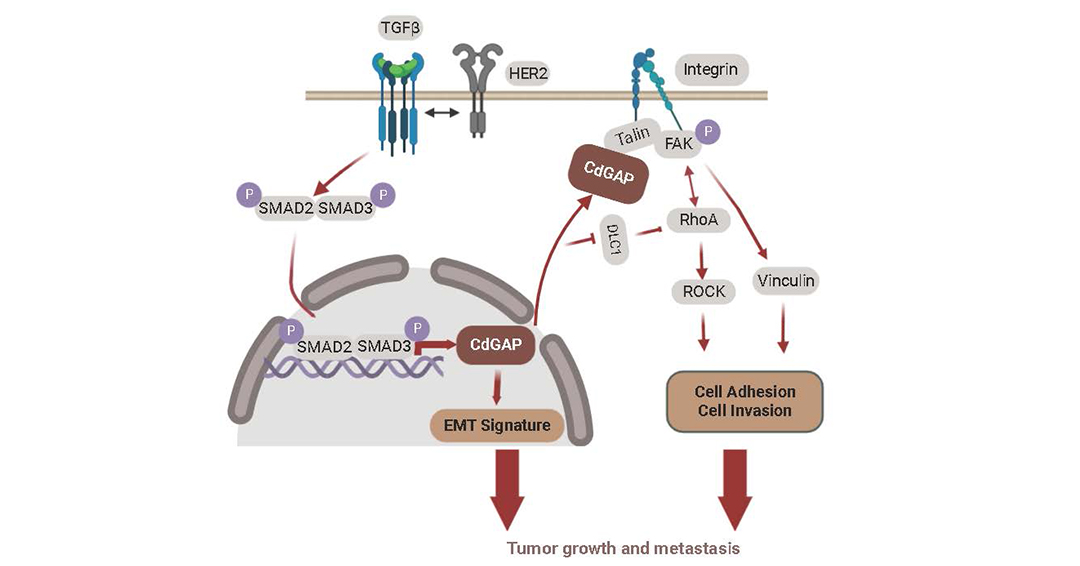
The research team showed that CdGAP is a molecular target of the TGF-β pathway, which, in turn, positively regulates an epithelial-to-mesenchymal transition (EMT) gene signature in HER2+ breast cancer cells. They were able to identify a crosstalk mechanism between CdGAP and the RhoA pathway through the tumour suppressor protein deleted in colorectal cancer 1 (Dlc1), a GAP inactivating RhoA. In addition, they uncovered the adaptor protein talin as a novel CdGAP protein interactor that modulates focal adhesion dynamics and integrin activation, leading to modulation of cell migration, invasion and adhesion, contributing to the aggressive metastatic progression of cancer cells. Furthermore, the authors showed that in patients, high CdGAP expression combined with a TGF-β-EMT signature is linked to disease progression.
“This publication is the result of seven years of effort and would not have been possible without the contributions of multiple teams with different areas of expertise,” says Lamarche-Vane. “Yi He drove this project with great enthusiasm, care and perseverance, working with Marie-Anne Goyette, PhD, formerly a trainee in the laboratory of Jean-Francois Côté at the Institut de recherches cliniques de Montréal (IRCM). This team generated the CdGAP HER2+ mouse model system together, discovering the major effects on tumour growth and metastasis. David Labbé, PhD, a scientist in the Cancer Research Program at the RI-MUHC and his research associate, Nadia Boufaied, PhD, offered expertise in RNA sequencing analyses that was instrumental in discovering the TGF-β-EMT gene signature and its association with the progression of the disease.”
About the study:
Read the publication “CdGAP is a Talin-binding protein and a target of TGF-β signaling that promotes HER2-positive breast cancer growth and metastasis” in Cell Reports
The authors gratefully acknowledge funding from the Canadian Institutes of Health Research.
The authors thank the Small Animal Imaging Labs (SAIL), the Proteomics and Molecular Analysis Platform, the Molecular Imaging Platform and the Histopathology Platform at the RI‑MUHC, and the Molecular Biology and Functional Genomics core facility at the IRCM.
