Understanding the mechanics of cardiopulmonary bypass
By Diane Weidner, Steinberg Centre for Simulation and Interactive Learning
A beating heart would be very messy and difficult to operate on. Thanks to a series of discoveries, experiments and innovations over the last century, this is not necessary. The heart can be temporarily stopped while a cardiopulmonary bypass (CPB) machine mimics the function of the heart and lungs, pumping blood and infusing the red blood cells with oxygen to keep the patient stable during surgery.
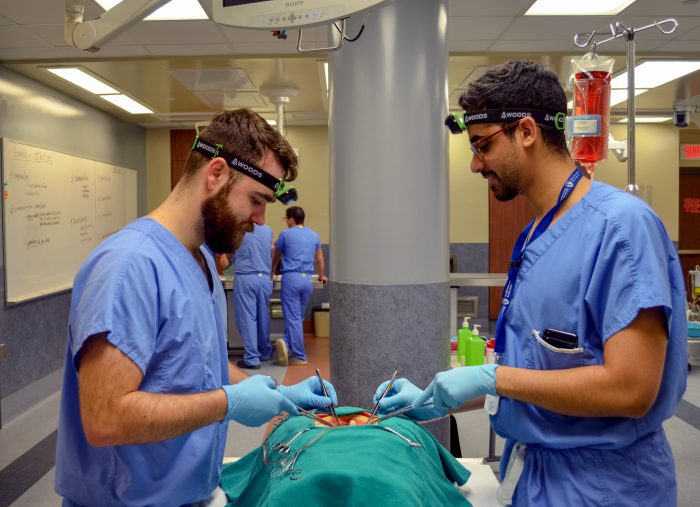
That being said, there are important steps to be mastered to ensure that everything runs smoothly during CPB surgery. This includes inserting and securing multiple cannulae into the patient’s body: a central venous cannula to remove oxygen-depleted blood, an arterial cannula to infuse oxygen-rich blood, and a cardioplegia cannula to deliver a solution that causes the heart to stop beating.
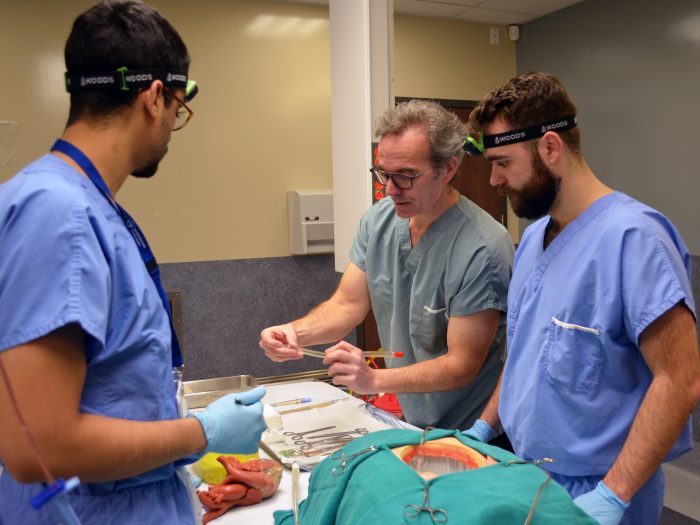
“The first time you insert a cannula into the aorta can be very intimidating, so the ability to practice this is key,” emphasizes Dr. Kevin Lachapelle, Professor of Surgery at McGill University who vividly remembers his first experience preparing a patient for this procedure. As the Founding Director and current Interim Executive Director of the Steinberg Centre for Simulation and Interactive Learning, he knows how important it is for learners to practice their procedural skills in a risk-free, simulated clinical environment, which is why he organized this half-day workshop for Junior Cardiac Surgery Residents at McGill.
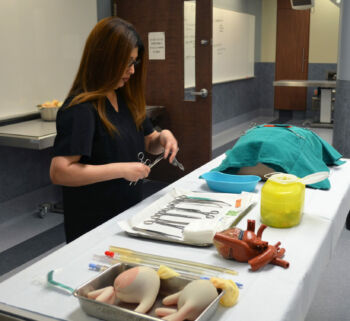
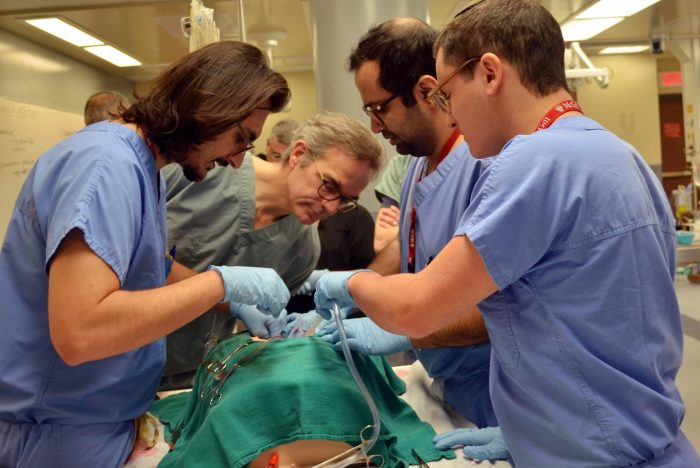
The residents may have observed CPB in the operating room, but they need to explicitly understand the process and be prepared to communicate and troubleshoot with the team. In small groups, they practiced hands-on cannula insertion and learned how to optimally orient and secure the cannula on simple but effective heart models created by Dr. Lachapelle and Surgical Skills Coordinator Simali Perera. The heart models were designed to mimic the texture of the ascending aorta and were created using low-cost materials – surgical gloves, fake tissue and artificial blood. The models were inserted into task trainers and connected to an IV, creating continuous blood flow and pressure to closely simulate realistic conditions for one of the most complicated organs in the body.
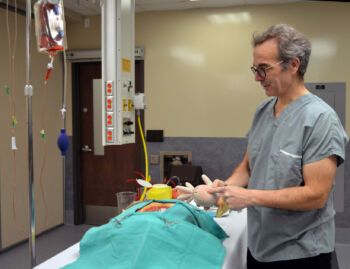
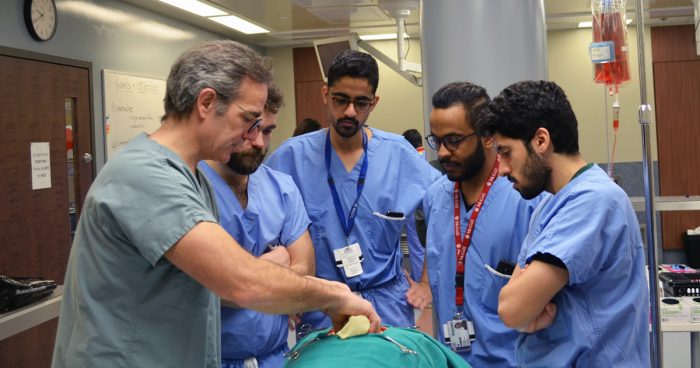
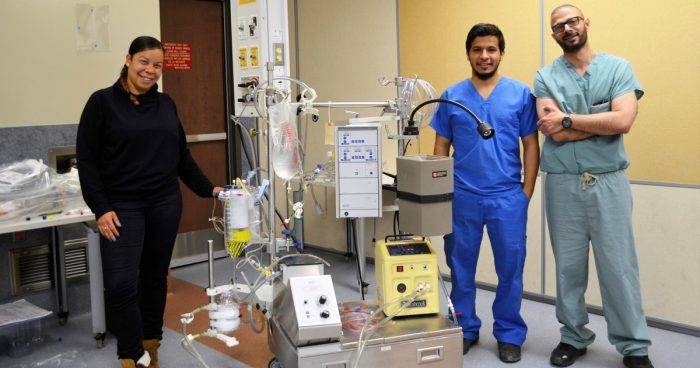
Another important objective of this interprofessional workshop was to provide residents with a solid understanding of the role of the cardiovascular perfusionist, a key member of the highly-specialized surgical team who operates the CPB machine and closely monitors the patient’s vital signs during open heart surgery. Jeanne Corriveau, a perfusionist from the McGill University Health Centre (MUHC) was joined by stagiaire Samuel Cormier, a perfusionist student from the Université de Montréal, to demonstrate the different sizes, shapes and flow characteristics of the cannulae and to discuss how to choose the right cannula for the right patient. “In 90% of the cases, this will be obvious, but your expertise is needed for the 10% that are the exception,” emphasized Dr. Lachapelle.

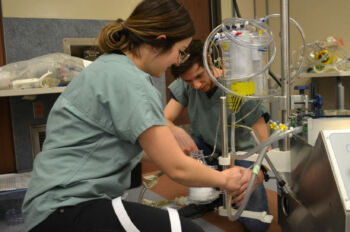
The residents gained an in-depth understanding of CPB machine from MUHC perfusionist Nissa Poisson-Thomas, who explained the technical process and provided insights on how the team can work together to manage different issues that may arise. “In the operating room, communication is key. We all have an important role to play. Just like the human body, we are a system and need to work together,” emphasizes Ms. Poisson-Thomas.
Everyone was so engaged that they did not want the workshop to end. “As Junior Cardiac Surgery Residents, this has been a very successful workshop. Being able to learn the techniques and principles of cannulation and the effect of teamwork in cardiac surgery is invaluable,” expressed Dr. Ziyab Sarfaraz.
Le 30 mars 2019