Medical student reflects upon his first experience working at a week-long ophthalmology clinic in Nunavik
For Indigenous people in remote communities, gaining access to healthcare services can be a challenge. In many cases, it means having to take long trips to urban centres, often by plane. Because this is not always a viable option, some people go without proper medical attention for conditions that are easily treatable.
To help address these challenges, Dr. Christian El-Hadad, Assistant Professor, Orbital Oncology, Ophthalmic Plastic and Reconstructive Surgery, in the Department of Ophthalmology and Visual Sciences, has been going Quebec’s Nunavik region six to eight times a year since 2020. “Together with local leadership support, we were able to redesign eye care in Nunavik, provide telemedicine services and most importantly change the offer of eye care from an itinerant model to a service-based model,” says Dr. El-Hadad.
Dr. El-Hadad says his work is a continuation of a decades-old tradition of ophthalmologists serving remote Indigenous communities. It is an initiative that is dear to his heart. “I have always been interested in humanitarian work and global health. I was introduced to Nunavik in a visit with Dr. Susan Lindley in April 2017,” he says. “Later in 2018, I learnt that there was a possibility to be the official ophthalmologist for Nunavik. I saw in this an opportunity to combine my profession with humanitarian work and aboriginal health.”
As part of that tradition, Dr. El-Hadad brings with him a medical student to assist with each clinic. In February 2022, Dr. El-Hadad travelled to Puvirnituq, Nunavik, to run a week-long clinic. He was accompanied by Jobanpreet Dhillon, a fourth-year medical student. We spoke to Dhillon about his experience. In the following interview, he discusses the challenges, the rewards and the takeaways from his time in Puvirnituq.
Tell us a bit about yourself, what program you’re in and what drew you to it.
My name is Jobanpreet Dhillon, and I am a fourth-year medical student at McGill University. Prior to medical studies, I completed an undergraduate in Interdisciplinary Medical Sciences followed by a Master’s in Biomaterials and Stem Cell Therapy at Western University. Although my interest in medicine flourished during undergraduate and graduate studies, I have always wanted to be in a profession where I could create sustainable impact in the health of the people in my community. Through medicine, not only am I able to form long-term meaningful relationships with my patients, but also be an advocate for change to bridge healthcare disparities. McGill Medicine has provided me with an excellent platform to exercise these principles while training to become a future physician.
How did you hear about the project in the north?
During my clinical elective in ophthalmology at the McGill Academic Eye Centre, I came to know an outstanding physician, surgeon and mentor, Dr. Christian El-Hadad. To learn about his work in organizing ophthalmic care for the Indigenous Peoples in Northern Quebec was both humbling and inspiring. While completing my research elective under Dr. El-Hadad, he was coincidentally scheduled to visit Puvirnituq, Nunavik, for another ophthalmic care assignment. He kindly offered me the opportunity to accompany him and learn about the intricacies of providing healthcare in a resource-limited setting. Needless to say, I jumped on this once-in-a-lifetime opportunity!
What made you want to get involved?
It was during my clinical experiences interpreting for the refugee and asylum seeker population when I learned more about the healthcare disparities among vulnerable populations in Montreal. Similarly, during my ophthalmology elective, I had the privilege of serving Indigenous patients in clinics. Hearing stories about their travels, wait times, and other challenges when seeking ophthalmic care, I became motivated to better understand the healthcare barriers that exist for this marginalized population. There was no better way to further my learning than immersing myself in the habitat and culture of the people from the remote Indigenous communities in Northern Quebec.
What did the day-to-day look like and what did you do?
My role was that of a clinical and surgical assist under the supervision of Dr. El-Hadad during this one-week experience in rural Nunavik. Through collaboration with the wonderful nursing team at the Innutsilvik Health Centre, we were able to service a high-volume Inuit patient population of all ages through daily surgeries and in-clinic assessments.

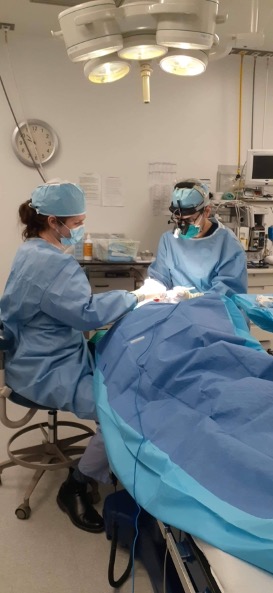
Every morning, I would arrive early at the hospital to prepare the operating room and daily clinics in conjunction with the nursing team. During the surgery, I would perform first assist duties with Dr. El-Hadad on specialized procedures such as dacryocystorhinostomies, blepharoplasties, and ectropion and entropion repairs. Additionally, I had the humbling opportunity to close skin incisions on the eyelids of a young Inuit patient. While the surgeries took place, the nursing team would triage the patients arriving for clinic appointments, who were seen in-between surgical procedures and during afternoon clinics. For these patients, I would perform comprehensive ophthalmic assessment, including visual acuity, intraocular pressures, slit-lamp and fundoscopy examination, and then relay my findings to Dr. El-Hadad.
The hospital had a small cafeteria with a very welcoming staff and great food options for lunch and dinner. Our living accommodations were comfortably located at a 2-minute walk away from the hospital in a 3-bedroom, 1-washroom unit with complete kitchen and laundry facilities. When the weather wasn’t too cold, Dr. El-Hadad and I were able to explore the small town of Puvirnituq in the evenings.
Any particularly memorable or surprising moments?
From experiencing the landscape of the remote town along the Hudson Bay to the vibrant culture of the Inuit Peoples, there were many memorable moments during this trip. However, one particular patient encounter certainly remains unforgettable!
Minutes before Dr. El-Hadad and I were set to depart for the airport to catch our return flight, a patient who recently underwent a dacryocystorhinostomy crossed paths with us at the hospital entrance in a panic. The wire-like silicone conduit that was keeping the nasolacrimal pathway patent post-surgery had displaced itself, causing it to protrude out of the eyelid. While this was visibly distressing for the patient, it also posed risk for improper healing and other complications. We rushed him to the hospital clinic and attempted to reposition the conduit; however, after multiple attempts, the best option remained to completely remove the conduit.
So why was this experience memorable? Well, other than the sprint race to the airport afterwards, this patient encounter perfectly highlights the barriers to ophthalmic care for this remote population. If we had not crossed paths, this patient would have had to wait weeks or months before getting access to a flight and coming down to Montreal to get the appropriate care. In that time, he could have developed infection and possibly compromised his vision in the affected eye. Or equally dangerous, the patient may have resorted to ‘fixing’ the problem himself to avoid the hassle of finding an English-speaking escort, travelling 5+ hours in a cramped airplane to Montreal, and staying in the city for several days away from family.
What did you learn through this experience?
This trip certainly allowed me to gain a better understanding of the commitment, resilience, and creativity it takes to organize clinical and surgical ophthalmic care suites in a remote setting. From the slow internet speeds that impeded efficiency of clinics to the limited availability of surgical instruments, a physician must be patient and adaptable in such a resource-limited environment. Not to mention, the support from the nursing team, hospital administration, and local counsel is paramount in ensuring the sustainability of such healthcare initiatives.
All these efforts cumulate to reducing some of the healthcare accessibility barriers for the Inuit population. Only through such experiences one realizes that the capacity and means to travel hundreds of kilometres to a well-equipped hospital is not equally feasible for all; old age, language barriers, personal responsibilities, and flying to an unknown city can all contribute towards limiting appropriate and timely ophthalmic care. Perhaps unsurprisingly, the Inuit People were extremely grateful and appreciative of receiving care in their own community and being able to return their home the end of the day, a privilege that we may take for granted.
In the future, I aspire to have a professional career that is inclusive in providing care for the marginalized and vulnerable populations in Canada. This experience has provided me with valuable insight into the steps and collaborations required to organize clinical and surgical care initiatives in rural settings. And I hope to utilize this knowledge during my residency to implement sustainable programs early in my career that brings awareness, education, and healthcare accessibility to the remote Indigenous communities of the North.
Would you recommend the experience to others?
Without a doubt, I would recommend this experience my fellow medical student colleagues and residents. They can expect to learn about how the broader determinants of health such as poverty, education, physical environment, social support, healthy behaviours, and accessibility can contribute to the healthcare disparities that exist among the vulnerable Inuit Peoples. Furthermore, it presents an incredibly unique opportunity to practice clinical and surgical ophthalmology in a resource-limited environment where one learns to adapt and improvise. Of course, this journey also offers the opportunity and privilege to experience a new culture and gain appreciation for the way of life of the Inuit Peoples.
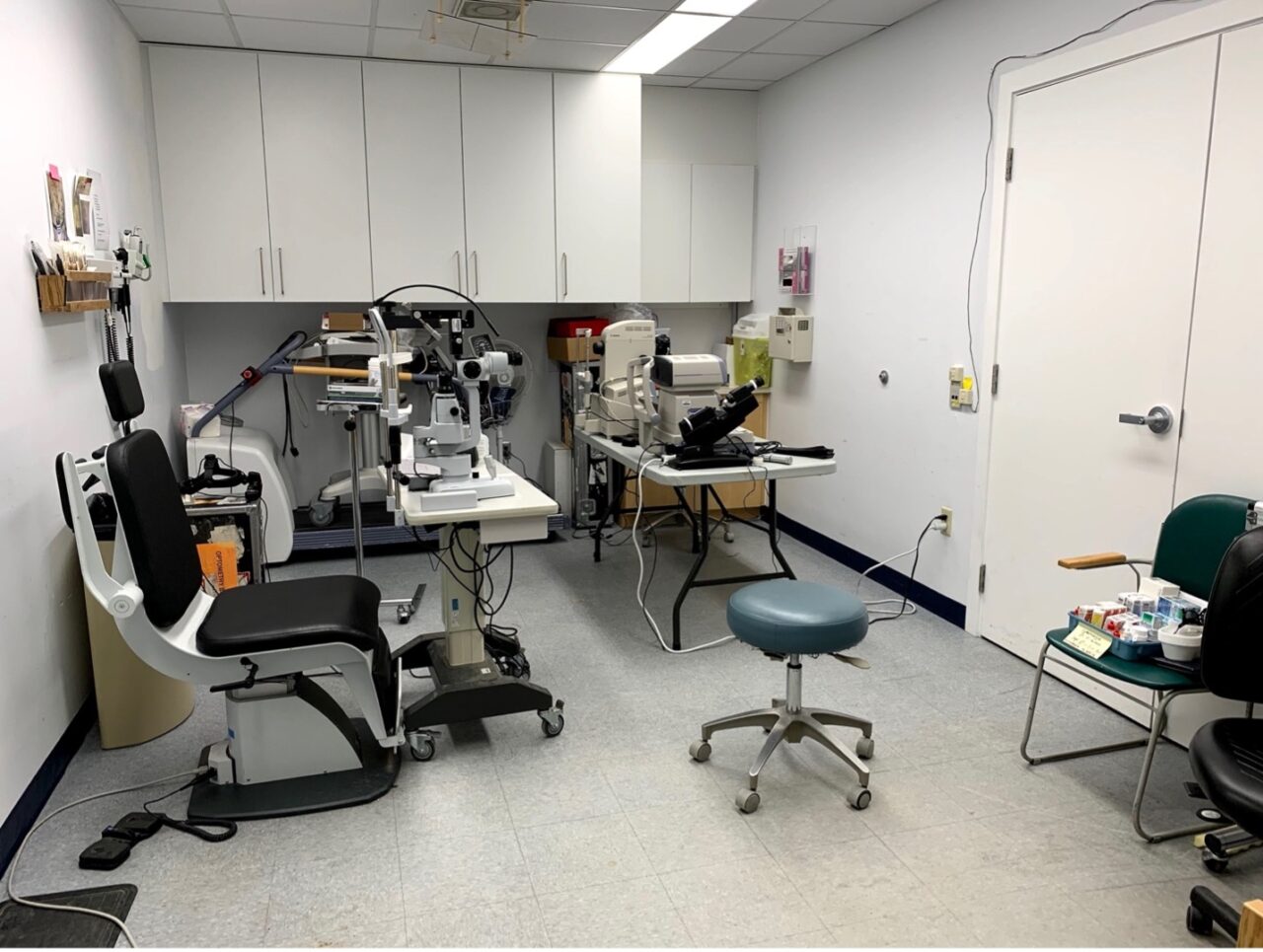
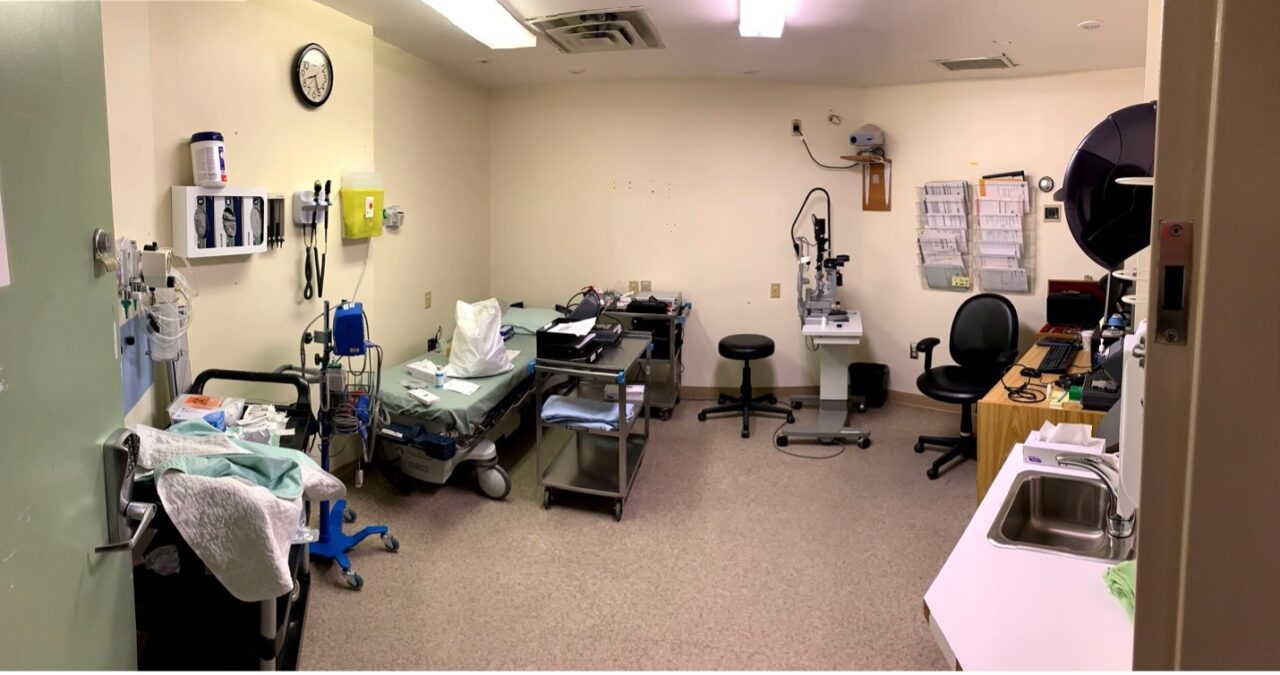
- Specialist clinic set as the Ophthalmology clinic for the duration of the Ophthalmologist’s visit at Ungava Tulattavik Health Centre, Kuujjuaq, Nunavik, Quebec.
- Canadian North airline – Kuujjuaq Airport, Boeing 737-200 Combi, Cargo compartment open to unload goods delivered from Montreal, QC
- Ungava Tulattavik Health, October 1st 2020, Kuujjuaq, Nunavik, Quebec
- October 2nd, 2020. The Northern village of Kuujjuaq, capital of Nunavik, Quebec
- October 2nd, 2020. The Northern village of Kuujjuaq, capital of Nunavik, Quebec
- January 16th, 2021. Runway – Kuujjuaq airport, Nunavik, Quebec
- Specialist clinic set as the Ophthalmology clinic for the duration of the Ophthalmologist’s visit at – Innutsilvik Health Centre, Puvirnituq, Nunavik, Quebec
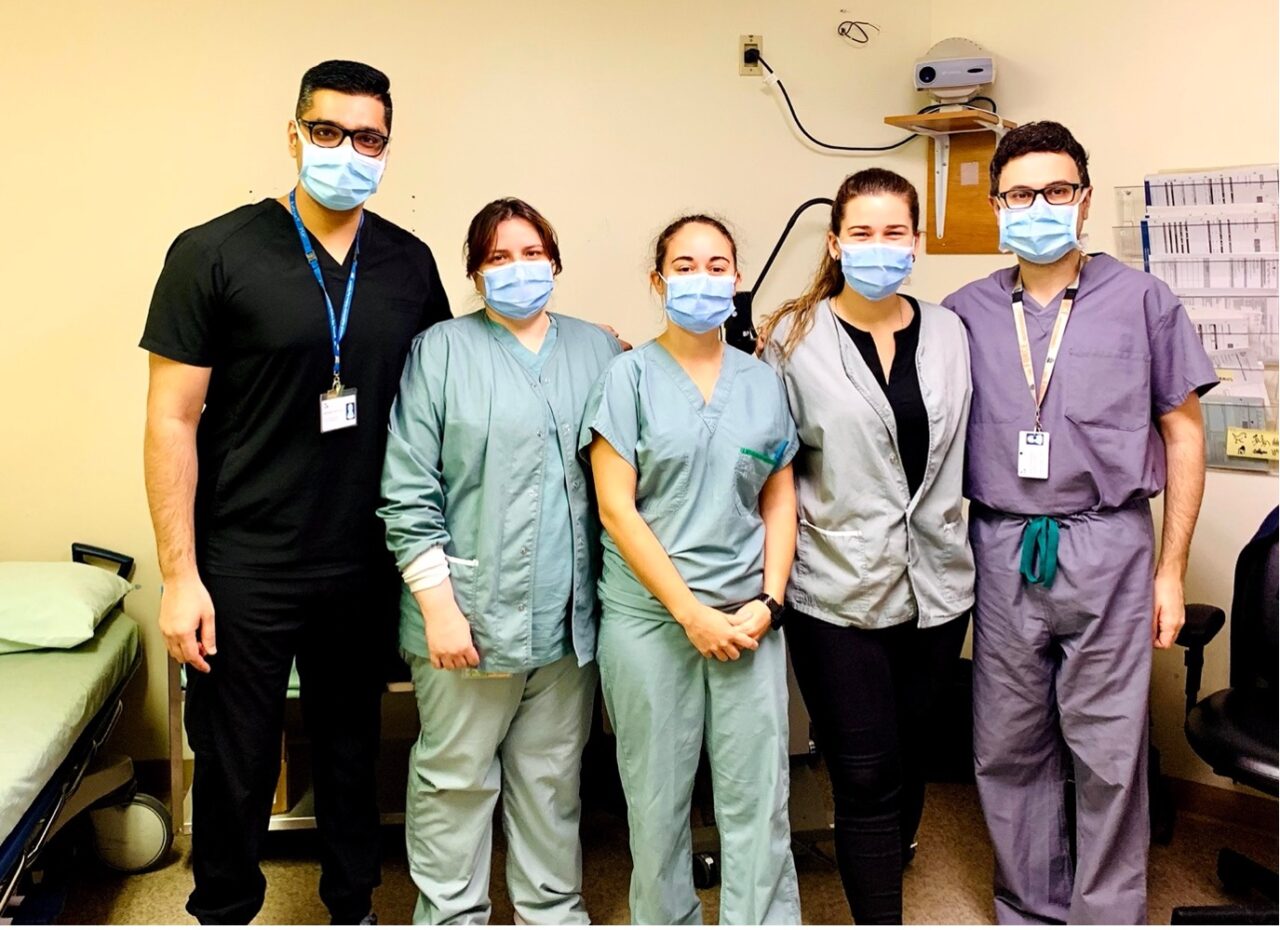
- Ophthalmology service team at the Innutsilvik Health Centre in Puvirnituq, Nunavik, QC. Medical student Jobanpreet Dhillon (left), sterilization technician, clinical and surgical nurses (middle), and attending ophthalmologist Dr. Christian El-Hadad (right).
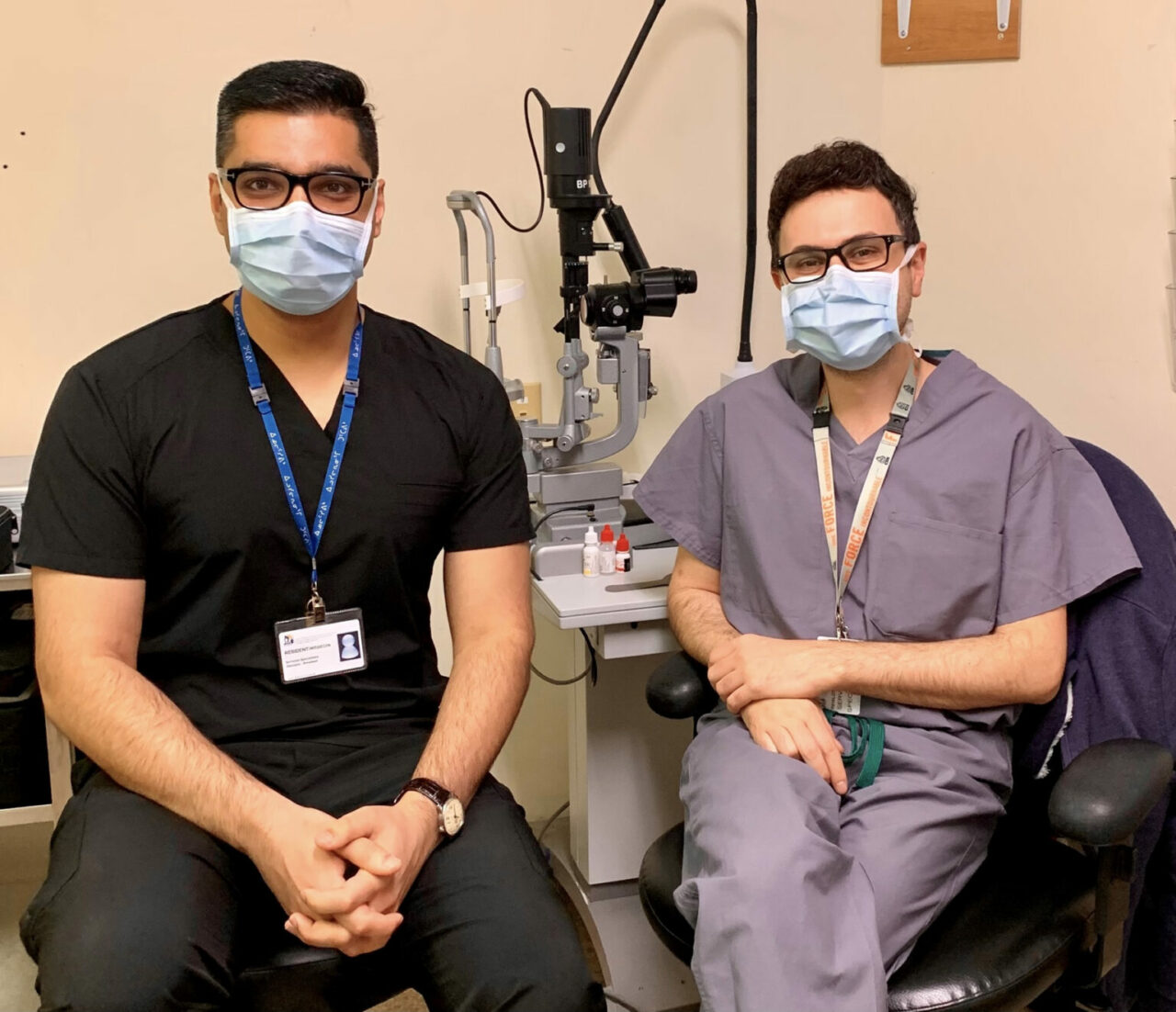
- Inuksuk – Kuujjuaq, Nunavik. Attending ophthalmologist Dr. Christian El-Hadad (left) and PGY-4 ophthalmology resident Dr. Ayman AlJohani (right).
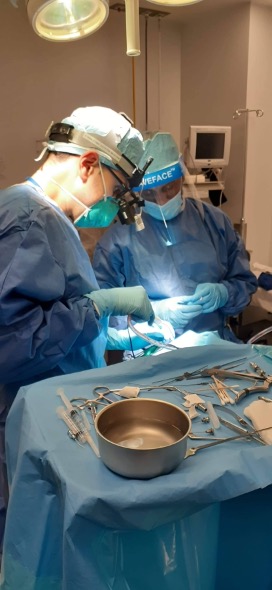
- Operating theater – Ungava Tulattavik Health Centre, Kuujjuaq, Nunavik, Quebec. Staff ophthalmologist Dr. Christian El-Hadad (left) and resident Dr. Ayman AlJohani(right) performing the first dacryocystorhinostomy (DCR) in Nunavik.
- Fuel Tanks, Kuujjuaq, Nunavik, Quebec.
- Specialist doctors housing, Puvirnituq, Nunavik, QC.
- Operating theater – Ungava Tulattavik Health Centre, Kuujjuaq, Nunavik, Quebec.
- Air inuit, Boeing 737 200C, Passenger Cabin, flight from Montreal Trudeau to Puvirnituq (interior view)
- Air Inuit, Beechcraft King Air 350, Flight from Puvirnituq to Kuujjuaq
- Air Creebec Departing from Kuujjuarapik, De Havilland Canada Dash 7 plane cabin in an Air Ambulance configuration.