Study of 84 countries links social trust and belonging to COVID-19 mortality

Source: McGill Newsroom
Trust in public institutions is linked to fewer COVID-19 deaths, but trust and belonging to groups is associated with more deaths, according to a wide-ranging, McGill-led study of 30-day COVID-19 mortality rates in 84 countries. Greater economic inequality is also associated with COVID-19 mortality.
The study led by McGill researchers published in Social Science & Medicine, is the first to show how global differences in COVID-19 mortality relate to income inequality. It also includes surveys on social trust and confidence in public institutions representing 86% of the global population.
The analysis reveals that COVID-19 mortality is linked to differences in trust. A lack of confidence in state institutions was associated with more deaths – consistent with research during the SARS and H1N1 pandemics. Surprisingly, however, the researchers found that social trust and belonging is also associated with mortality. While connecting with friends and family is a natural response in times of crisis, in some countries, this trust and the desire to socialize may be interfering with efforts to contain transmission through physical distancing.
Moreover, strong group bonds can sometimes reinforce risky health behaviours, so that high-trusting societies may be more susceptible to misinformation about the severity of COVID-19, bogus treatments, or dismissive attitudes towards physical distancing. “People expect there are health benefits to trusting others and belonging to groups – and there usually are. But in the context of a pandemic, when you need people to self-isolate, blind trust in others can get in the way,” says lead author Frank Elgar, a professor at McGill University and Canada Research Chair in Social Inequality in Child Health.
On the other hand, confidence in public institutions and civic participation were linked to fewer deaths, possibly because they mobilise people to wear masks, wash their hands, and practice physical distancing. The researchers note that being engaged in the community is particularly beneficial when groups are asked to compromise some personal freedom for the common good, like wearing a mask in public.
“Governments and other organisations can capitalise on this engagement during a pandemic by supporting safe ways for people to socialise and remain involved in their communities and cultural activities.”
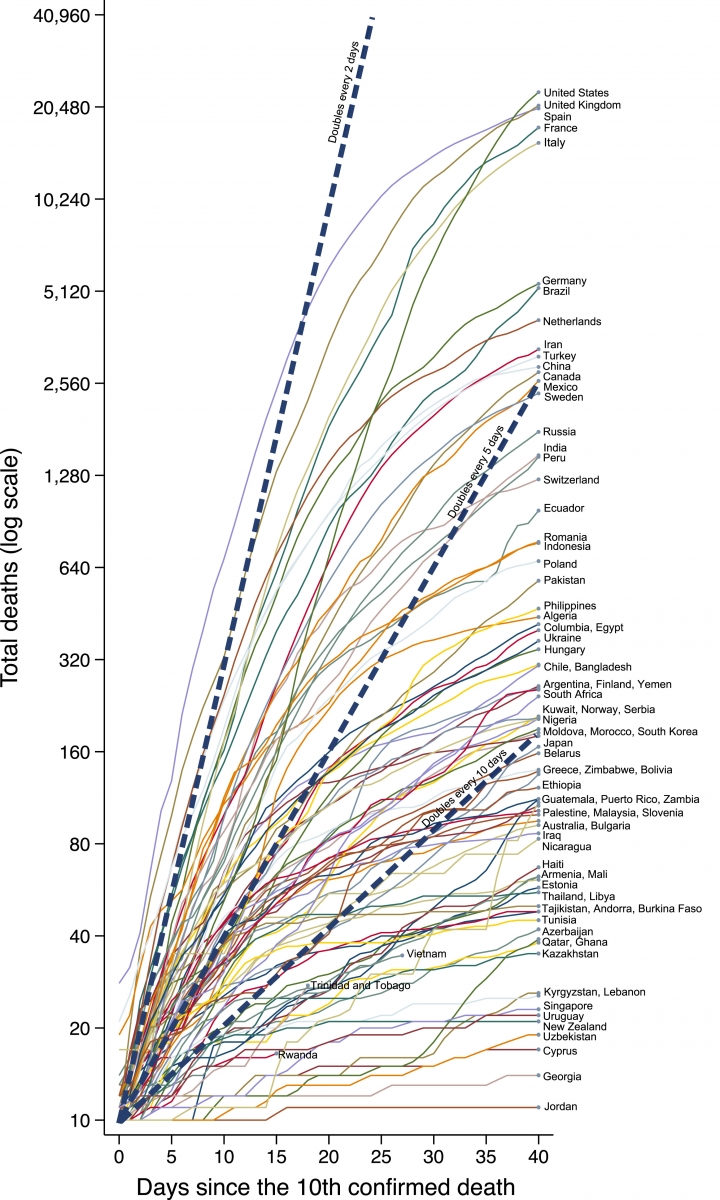 Inequality, not just poverty, a health problem during the pandemic
Inequality, not just poverty, a health problem during the pandemicThe researchers also found that income inequality is associated with more deaths, even after accounting for other social factors like national wealth and population age. “Countries with a larger gap between rich and poor, like the United States, Russia, and Brazil are experiencing a more deadly pandemic,” says Elgar, who is also a member of the Department of Psychiatry in the Faculty of Medicine.
“In many countries, lower-wage workers are over-represented among the essential workers in retail, public transit, and health care settings who cannot easily practice physical distancing,” says Elgar. Greater exposure to the virus and less access to health services among the poor could explain why more economically unequal countries – not necessarily the poorest countries – experienced significantly higher mortality rates. The researchers note, however, that wealthier countries may also have more accurate data or shorter lags in supplying death counts to health officials.
“There is a serious message here about the new challenges we will likely face in this second wave of the pandemic, and our capacity to mount a defense,” says Elgar.
“The trouble with trust: Time-series analysis of social capital, income inequality, and COVID-19 deaths in 84 countries” by Frank Elgar, Anna Stefaniak, and Michael Wohl is published in Social Science & Medicine.
DOI: https://doi.org/10.1016/j.socscimed.2020.113365
October 7 2020
