October is Brain Tumour Awareness Month
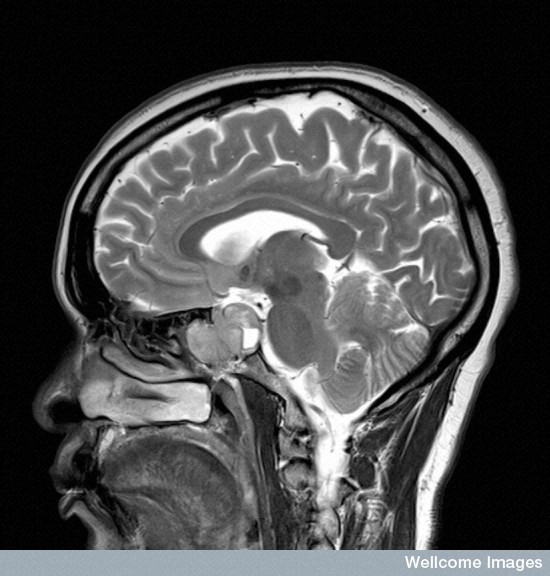
Every day, 27 Canadians are diagnosed with a brain tumour and an estimated 55,000 Canadians are surviving with a brain tumour. The most common type of primary malignant brain tumour is glioblastoma multiforme (GBM). Average survival, even with aggressive treatment, is less than one year. At the Montreal Neurological Institute and Hospital (The Neuro) at McGill University and the McGill University Health Centre, scientists and physicians are dedicated to combining the best possible treatment of patients suffering with brain cancer with state of the art research.
The Neuro-Oncology Program is the only adult centre in Quebec to achieve a Level 4 accreditation rating (the highest possible rating) from the Province. Over 3,000 patient visits in the Neuro-Oncology Clinic annually. The interdisciplinary team of 14 professionals including surgeons, nurses, oncologists, rehabilitation therapists, and a social worker, has made significant contributions to improving the care of individuals and families experiencing brain tumours.
The Neuro’s Brain Tumour Research Centre integrates the best possible clinical care with front-line research. 8 principal investigators work full time with more than 70 students, trainees and laboratory personnel to identify new, promising agents and strategies in the laboratory and ensure that they are brought quickly to the patients who need them.
Ultrasound-MRI
An improved brain scanning technique for neurosurgeries has been developed by Dr. Louis Collins and colleagues in the McConnell Brain Imaging Centre. The technique merges ultrasound and magnetic resonance imaging (MRI). Using ultrasound in brain operations, makes is possible to distinguish normal healthy brain tissue from tumours, but sometimes these images can be difficult to interpret. To address this, Dr. Collins and his team developed a way to correlate intra-operative ultrasound images with pre-operative MRI scans. This provides a more precise map when navigating tumour removal during surgery.
A new surgical tool, called fluorescence-guided resection, could dramatically increase the efficacy of brain cancer surgery. A metabolite known as 5-ALA, is administered to the patient. When 5-ALA is metabolized, one of its by-products is fluorescent. This metabolic pathway is more active in cancer cells making them more fluorescent – hence, distinguishable from normal brain cells.” This is especially useful in distinguishing the border between cancerous tissue and healthy tissue, which helps surgeon’s perform a more complete tumour resection and avoid damaging critical brain areas during the surgery.
Putting genetic brakes on brain tumours
“The way to stop the spread of brain cancer cells is to inhibit gene expression,” says neurosurgeon Dr. Kevin Petrecca. Years of testing and research have led to a precise gene therapy approach that Petrecca describes as “a switch that prevents brain cancer cells from spreading.” The Neuro’s team artificially engineered a molecular agent and introduced it first into cancer cell culture models and then into pre-clinical models. In both cases cancer cell movement was stopped. The team is moving towards bringing this therapy into a clinical trial.
Dr. Anita Bellail and colleagues have shown that a member of the protein family known as SUMO (small ubiquitin-like modifier) is a key to why tumour cells multiply uncontrollably, especially in the case of glioblastoma, the most common and lethal brain cancer. The SUMO family proteins modify other proteins and the SUMOylation of proteins are critical for many cellular processes. Identifying SUMO’s role in the cancer cell growth will lead to a new strategy for glioblastoma treatment.
Dr. Stefano Stifani and colleagues have identified two specific key players in the growth of GBM. A GBM tumour contains a complex combination of different cell types, including ‘stem-like’ cells that are able to initiate brain tumour growth, even when present in very small numbers. These cells, known as brain-tumour initiating cells (BTICs), are believed to be among the cells that can re-initiate GBM if they are not completely eradicated through surgery, radiation and chemotherapy. The implication of transcription factors FOXG1 and TLE in the tumour-forming ability of BTICs opens the door to possible strategies to block tumour growth – a major advance in the fight against GBM.
The creation of reliable biomarkers for use in the treatment of high-grade brain tumours is currently sought through dynamic contrast-enhanced magnetic resonance imaging (DCE MRI). However, the biological significance of the data generated by this technique is often difficult to interpret and there is a high failure rate due to technical challenges. Arterial Spin Labeling (ASL) Perfusion MRI offers distinct advantages over DCE MRI, but experience with ASL MRI in brain tumours is limited. A project by Dr. Barry Bedell compares ASL and DCE MRI technology via imaging studies of 10-15 patients with suspected, high-grade cerebral glioma. The data from this study will indicate whether ASL can replace the existing method or whether it supplies different, complementary information and could be used in tandem.
The Montreal Neurological Institute and Hospital — The Neuro, is a unique academic medical centre dedicated to neuroscience. Founded in 1934 by the renowned Dr. Wilder Penfield, The Neuro is recognized internationally for integrating research, compassionate patient care and advanced training, all key to advances in science and medicine. The Neuro is a research and teaching institute of McGill University and forms the basis for the Neuroscience Mission of the McGill University Health Centre. Neuro researchers are world leaders in cellular and molecular neuroscience, brain imaging, cognitive neuroscience and the study and treatment of epilepsy, multiple sclerosis and neuromuscular disorders. For more information, visit theneuro.com.
October 3, 2014
