The family of Edith Levy, MDCM’42, was planning for her 100th in June when she passed away on March 24, 2018.
Was she the oldest living MDCM, they wonder.
And to what might she have owed her longevity, we ask.
Athletics and social skills,” says daughter, audiologist Joyce Stein, BSc’65, MSc(A)’67. “My mother was a social animal and she kept herself very active. She had a million friends and took care of them all.”
Hailing from New Orleans, Levy started her medical training at Louisiana State University, where she was one of two women in the class. When she transferred to McGill, it was to the Medicine class with the largest female cohort in the history of the Faculty. The ten coeds formed a close bond. “In the summer, they all did a rotation together at the Montreal Maternity,” says Stein.
At graduation, Levy took the Campbell Howard Prize in Clinical Medicine, ranking in the top ten of her class. She did not go into medical practice, one of her life’s few regrets— and, points out VP-Dean David Eidelman, MDCM’79, a reflection of the challenges faced by Levy’s generation of women physicians. “Someone like her who graduated at the top of her class could have run her own laboratory,” he says, “rather than simply being a team member.” As it was, she worked in the blood lab of fellow Southerner Dr. Louis Lowenstein, studied heart sounds with Harold Nathan Segall, MDCM’20, DSc, and conducted pioneering Alzheimer’s research at the Jewish Hospital of Hope with former classmate, Bob Levine, BSc’40, MDCM’42, DIP SURGERY’51.
Levy, who was married at 21 and expecting by convocation, leaves behind ten grandchildren and 19 great-grandchildren. Two of her grandkids are McGill-trained doctors, Robert Stein, BSc’93, MDCM’97, PGME’00, and Alison Stein, MDCM’98, as is her son-in-law, Lawrence Stein, BSc’64, MDCM’68. Her son David Levy, DSc, is a famous astronomer who has discovered many comets and asteroids, including Asteroid Edithlevy, named in her honour.
Joyce explains that her mother lived the good life for virtually ten decades by being physically, mentally and socially active at each stage. Levy sailed and played lots of golf, still hitting the greens well into her 90s. She enjoyed her family and was always surrounded by people, whether at the club or with her bridge group.
She also continued to educate herself. “She took courses at McGill later in life to go back to work at the Montreal Children’s Hospital in genetics.” There, she worked alongside one of the creators of the field, F. Clarke Fraser, MSc’41, PhD’45, MDCM’50, DSc.
Of her colleagues, Segall would live to 101, Levine, to eight days shy of 99, and Fraser, to 94.
Although a stroke a few years ago had slowed Levy down considerably, she still went, this winter, to the gym in her building twice a week with physiotherapist Mina Tehila Schacter, BSc(PT)’99, to put in her twenty minutes on the stationary bike.
Levy gave this advice to her grandchildren at age 86: “There are some lessons learned from a long life and wisdom that comes from age. Appreciate the importance of family and keep the family ties strong. Be there for all the special occasions and the not-so-special occasions.” A life well lived will pay dividends through the generations. “Don’t be afraid to give your children guidance. Set an example in how you choose to live. Try to be someone of whom they can be proud,” she said.
For those of us who are inspired by Levy and others of her ilk, what factors are scientifically known to contribute to longer, happier and healthier lives? To find out, Medicine Focus invited a panel of clinicians and researchers to weigh in with some evidence-based advice.
1. What’s good for your heart is good for your brain.
 It turns out that the lifestyle prescriptions that keep your heart healthy are just as important for boosting your brain health, and in helping to prevent or delay the onset of Alzheimer’s disease (AD). According to Dr. Serge Gauthier— Director of the Alzheimer’s Disease Research Unit at the McGill University Research Centre for Studies in Aging, Douglas Mental Health University Institute—and Dr. Pedro Rosa-Neto—a clinician scientist at the Douglas and Acting Director of the Centre—research shows that ongoing physical, mental and social activities have protective cognitive benefits. Being active in these ways were hallmarks of Edith Levy’s life from her youth through middle age and into her 90s.
It turns out that the lifestyle prescriptions that keep your heart healthy are just as important for boosting your brain health, and in helping to prevent or delay the onset of Alzheimer’s disease (AD). According to Dr. Serge Gauthier— Director of the Alzheimer’s Disease Research Unit at the McGill University Research Centre for Studies in Aging, Douglas Mental Health University Institute—and Dr. Pedro Rosa-Neto—a clinician scientist at the Douglas and Acting Director of the Centre—research shows that ongoing physical, mental and social activities have protective cognitive benefits. Being active in these ways were hallmarks of Edith Levy’s life from her youth through middle age and into her 90s.“Physical exercise is the best for prevention. But education and keeping your mind active throughout life, especially after retirement, and social interaction are also important, especially in strengthening brain resilience or brain reserve,” says Gauthier. Some recent studies have even shown that aerobic exercise may reduce the levels of tau and amyloid proteins, which accumulate in the brain and damage it to cause AD, says Rosa-Neto.
Gauthier sees special advantages in doubled-barrelled activities, like belonging to a book club, compared with just reading on your own. “You get the mental stimulation and the social interaction in a book club, which is as important as what you read,” he explains. Avoiding chronic stress has preventive benefits too. “Chronic stress damages the brain’s memory system, accelerates aging and contributes to the development of AD,” explains Rosa-Neto.
A key research goal of the Centre for Studies in Aging is to focus more intensively on personalized interventions to prevent or treat people in the pre-clinical phase of AD, where the person has harmful tau or amyloid proteins accumulating in the brain, or vascular changes, but no symptoms.
“Lifestyle interventions are important for everyone,” says Gauthier. “However, since the relative weight of various pathophysiological components of AD will be different over time and will even change over time for each individual, a ‘one drug fit for all’ approach is no longer defensible. Precision medicine using biomarkers in the diagnosis and treatment of AD is the new strategy. We’ll do smaller clinical trials that target high-risk patients before they have symptoms and we’ll know within two years whether the drug works,” he says.
Studies show that education in childhood can impact levels of cognition decades later. Neuroscientist Lesley Fellows, BSc’90, MCDM’96, PGME’01, suggests there is a strong social justice argument for investing in childhood education to prevent brain health issues later. “What’s good for your mind is good for your brain. High educational attainment may be good for your brain, in that it is associated with a lower risk of cognitive decline in later life,” says Fellows, Assistant Dean, Academic Affairs, and Professor in the Department of Neurology & Neurosurgery, adding that, from a policy perspective, it makes sense to start planning for healthy aging from early childhood on.
Your brain also thrives on meaningful interactions and connections with a huge hive of family, friends and community. “The bigger your social network, the more you use your social brain.” Social support and social relationships, the more of these you have, the better off you are, says Fellows.
3. Keep your voice in optimal condition by drinking lots of water and resting it when you’re sick.
“Don’t take your voice for granted,” says Tara Casorso, MSc(A)’16, noting people often don’t pay attention to their voice until they develop a problem. “For humans, our voice is one of our main avenues for communication and social connection, so taking care of it is very important to our well being,” says Casorso, who works as a Speech-Language Pathologist with Island Health in Victoria, British Columbia.
Research shows some voice problems can be caused by changes due to aging, such as shrinking of the muscles, stiffening of the ligaments, or changes in respiratory function. But Casorso offers a few practical, preventive tips to help keep your voice in optimal condition: “Warm up your voice in the morning with simple exercises that include humming, gliding from a high pitch to a low pitch and vice-versa, and lip/tongue trills. Cool-down exercises that you can do in the evening relax the vocal muscles and include yawning, humming and sighing. Also, get lots of sleep. Our vocal muscles and tissues are rested and repaired during sleep,” says Casorso.
4. As calorie requirements fall with age, especially after 50, and nutrient needs stay the same, eat a more nutrient-dense diet and fewer “free calories” that accumulate as fat.
Healthy eating, along with regular physical activity, is key to maintaining a healthy weight and reducing the risk of metabolic syndrome, advises José Morais, PGME’94, Director of the Division of Geriatric Medicine, School of Dietetics and Human Nutrition, Department of Experimental Medicine, and Associate Director, Quebec Network for Research on Aging. “The characteristic features of metabolic syndrome—large waist, hypertension, abnormal cholesterol profile and elevated blood glucose below the threshold for diabetes—are a well-recognized risk factor for heart disease and the development of diabetes. Metabolic syndrome also affects mobility when body mass is above 27 kg/m2. One simply cannot maintain a healthy weight without controlling dietary intake,” says Morais.
Wise dietary choices evolve as we age, however: “In middle age, one needs to reduce caloric intake to prevent obesity. At an advanced age, one needs to maintain intake to prevent weight loss, a condition contributing to frailty.”
The wide-ranging benefits of eating a healthier diet and being more physically active were demonstrated in research by Morais and collaborators in the Quebec Longitudinal Study on Nutrition and Successful Aging, aka the NuAge Study. “Those participants who were more physically active and eating a healthier diet were less likely to lose muscle mass over three years. They were also more likely to maintain better physical performance in tests such as gait speed and chair rising capacity, perform better in cognitive tests and have better mood,” he says.
Recent advances in cancer metabolism research also suggest that too much insulin in the blood, common in obesity, can promote tumour growth. Eating too much sugar can lead to high insulin levels. Metabolism researcher Michael Pollak, MDCM’77, advises the best approach to sugar is to think of it like spice. “Sprinkle sugar occasionally on foods, as opposed to having it as an ingredient in nearly every meal and too many drinks,” says Pollak, Director, Division of Cancer Prevention, Gerald Bronfman Department of Oncology, and Alexander Goldfarb Research Chair in Medical Oncology.
5. Maintaining strong social connections with your family, friends and primary care physician is good for your physical health and emotional and mental well-being as you age.
 Dr. Shamiel Alexis McFarlane, an MSc candidate in Family Medicine, examined the role and attitudes of primary care physicians in improving access to care and the health outcomes among the socially isolated elderly in rural Jamaica for her thesis project.
Dr. Shamiel Alexis McFarlane, an MSc candidate in Family Medicine, examined the role and attitudes of primary care physicians in improving access to care and the health outcomes among the socially isolated elderly in rural Jamaica for her thesis project.“I want to implement a pilot project to create an accredited community outreach program that would take physicians to isolated older people in the community and the physicians would earn the credits needed to renew their license,” says McFarlane, who plans to specialize in geriatric medicine.
While practicing as a family physician in Jamaica for eight years before coming to McGill, McFarlane saw firsthand the strong links between social connectedness and physical health. “The longer I was in practice, the more I saw that social issues had just as much impact on my patients’ physical and mental well-being as physical issues. If you’re interested in healthy aging and not being isolated, expand your social network early in life. You’ll benefit when you’re 75 and your kids and grandchildren live three provinces away,” she says.
6. Draw on the support of family, friends and nurses to help navigate the health care system while managing chronic or multiple illnesses.
In her dissertation, Fay Strohschein, MSc(A)’05, is exploring treatment decision-making from the perspective of older adults with colorectal cancer. Her study findings highlight the ongoing importance of trust in the health care system for patients as they entered and moved toward treatment. “The trust was shaped both by their interactions with health care providers and their experiences of the health care system. Those experiences, along with the help they often received from family and friends, determined whether or not they chose to trust and received, or continued receiving, treatment,” says Strohschein, a PhD candidate at the Ingram School of Nursing and nurse navigator for senior oncology patients at the Jewish General Hospital.
Nurses play a critical role in supporting the quality of life of older adults in coping with chronic illness. “The rhythms that our health care system imposes on people can be as disruptive as the illness itself, particularly for people managing multiple chronic illnesses. Nurses are often uniquely positioned to address concerns across multiple domains (physical, psychological, social) that can impact well-being. We play an important role in helping patients and families negotiate the health care system, coordinating and integrating care among “ interprofessional team members,” says Strohschein.
Sara Ahmed, BSc(PT)’96, MSc’98, PhD’04, conducts research aimed at improving health outcomes for people with chronic disease. “Chronic illness, as opposed to a short-term acute condition, requires individuals to learn the skills needed to manage their health over the long run. Studies show individuals who learn these skills are likely to be more confident to do the things they need to do to better manage their health, like taking medications as prescribed, staying physically active and seeking help when they need it,” says Ahmed, Associate Professor, School of Physical & Occupational Therapy (SPOT).
Her research studies on self-management interventions for asthma, chronic obstructive pulmonary disease (COPD), acquired brain injury and chronic pain have shown the importance of tailoring interventions to individuals’ specific needs and the benefits of e-health tools. “E-health solutions can improve disease-specific quality of life by providing the tools to monitor their symptoms and stay connected with their care providers. Monitoring and ongoing communication with the care team helps patients receive recommendations, rather than waiting for a visit at the clinic. This can help prevent exacerbations or deteriorations in health that may result in an emergency department visit and reduced physical and mental health function,” she says.
8. Stay active and healthy, accept outer changes and beware of “magic bullets.”
Bioethicist Jennifer Fishman is all in favour of people aging well. But she has ethical concerns about claims and assumptions made by certain anti-aging practitioners, who promote quick-fix drugs and supplements to reverse aging and extend life. “There are questions about the safety and efficacy of long-term hormone replacement therapy for life extension, for example, and we really don’t know enough about long-term effects that could possibly be harmful to health. I don’t fault anyone for looking for a magic bullet, but the money spent on these products could be used to do other things that would give people a better quality of life,” says Fishman, Associate Professor in the Biomedical Ethics Unit and the Department of Social Studies of Medicine.
Fishman cautions that some implicit assumptions in anti-aging or successful aging marketing can discourage people from a healthy acceptance of normal aging. “There is an ageist element to the successful aging movement, which suggests there’s a problem with growing old. It assumes we have total control over the aging process, which we don’t, and it may encourage us to blame people who don’t age well because they didn’t do the right things,” she says.
Gerontologists should encourage older adults to stay active and vital, maintain mobility, and accept the outer changes that come with aging. “The golden ticket would be compressed 35 morbidity, so you extend quality of life and reduce time spent ill later in life. Another essential social goal is to create a society that is more accepting and accommodating to an aging population,” she says.
 Patricia Belchior, Associate Professor, SPOT, evaluates the effectiveness of video-game training in improving the visual attention skills of older adults. “Research has shown certain types of computer and video games can improve some aspects of cognitive skills among older adults. For instance, our research on visual attention has used games that have certain characteristics, such as the need to react to unpredicted stimuli on the screen and being fast-paced,” she says.
Patricia Belchior, Associate Professor, SPOT, evaluates the effectiveness of video-game training in improving the visual attention skills of older adults. “Research has shown certain types of computer and video games can improve some aspects of cognitive skills among older adults. For instance, our research on visual attention has used games that have certain characteristics, such as the need to react to unpredicted stimuli on the screen and being fast-paced,” she says.More broadly, Belchior offers this advice for aging well to people living with or without disabilities: “Keep active by playing a sport, dancing or walking. Keep challenging your brain by learning a new language, learning how to play an instrument or learning a new skill. Keep social and engage in occupations that are meaningful and bring you satisfaction. And above all, keep a positive attitude towards the aging process,” she says.
10. Set SMART goals to increase your motivation for exercising and gain specific mobility benefits that matter in your daily activities.
As a co-investigator in the pilot study Managing Mobility Outcomes in Vulnerable Seniors (MMOVeS), Sabrina Figueiredo, MSc’10, PhD’17, observed the benefits of a six-month, individualized, exercise-focused, self-management program in improving mobility for seniors after a hospital discharge. “Our findings suggest participants in the MMOVeS group had three times greater odds of improving in any of the seven mobility indicators than participants in the exercise information group,” says Figueiredo, Assistant Professor, SPOT, and Associate Director of the Physical Therapy Program.
Figueiredo believes that adding behavioural strategies to physical exercise programs can get older adults to stick with them and reap the benefits in their daily lives. “Sometimes patients have difficulty in grasping how isolated exercises will improve their performance of daily activities. Adding goals to your exercise routine may increase your motivation to keep exercising. For this to be successful, you need to set SMART goals, which are specific, measurable, attainable, realistic and have a timeframe for accomplishing them,” she says.
Prevention of mobility limitations with aging should start early in life. “Just as young adults are encouraged to invest in a bank retirement plan for the years to come, they should be encouraged to invest in physical fitness during their peak capacity to benefit from the positive effects of exercising as the body ages,” says Figueiredo.
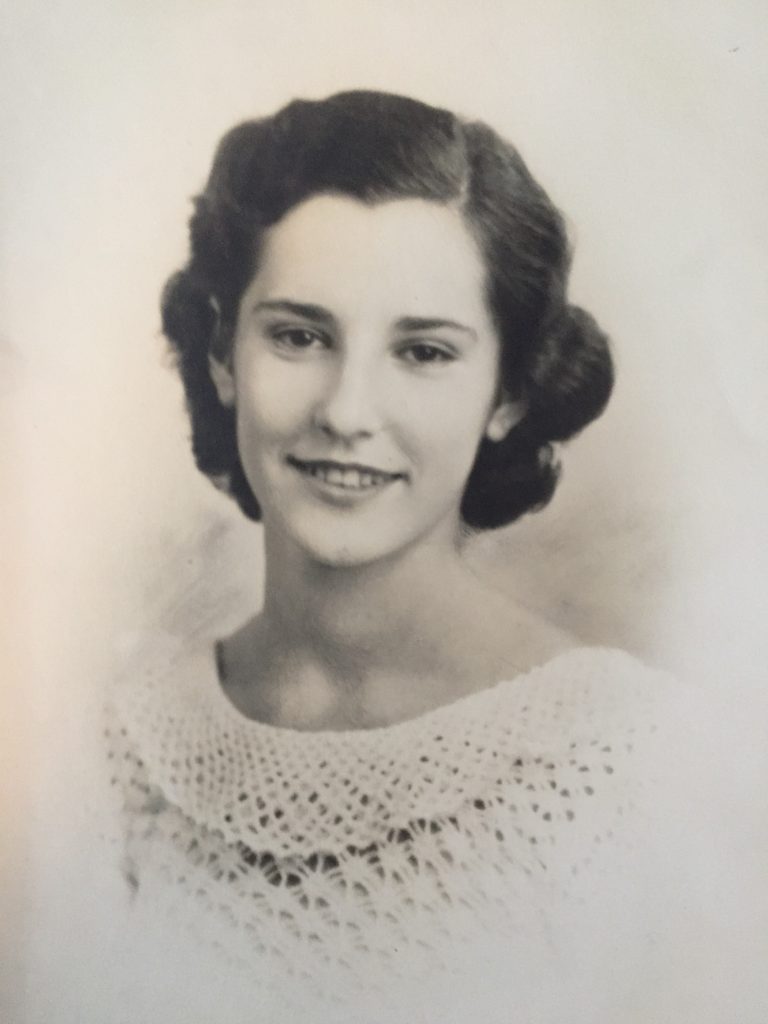 Young Edith Levy was so invested in physical fitness and social camaraderie that she swam in the U.S. Olympic trials at 17. In the short term, she was denied the opportunity to compete in the 1936 Berlin Olympics because of Hitler. “All the Jewish athletes pulled out of the team, so she never got to go,” says her daughter Joyce Stein. But Levy reaped the long-term benefits of being physically and socially active throughout her life until her final days. Stroke aside, Stein attributes her mother’s relatively good health up until the very end to a lifetime love of activity. “She was never not doing something and then her physiotherapist kept her moving!”
Young Edith Levy was so invested in physical fitness and social camaraderie that she swam in the U.S. Olympic trials at 17. In the short term, she was denied the opportunity to compete in the 1936 Berlin Olympics because of Hitler. “All the Jewish athletes pulled out of the team, so she never got to go,” says her daughter Joyce Stein. But Levy reaped the long-term benefits of being physically and socially active throughout her life until her final days. Stroke aside, Stein attributes her mother’s relatively good health up until the very end to a lifetime love of activity. “She was never not doing something and then her physiotherapist kept her moving!”
July 30, 2018

