 RI-MUHC-led study compares saliva self-test to blood test
RI-MUHC-led study compares saliva self-test to blood test
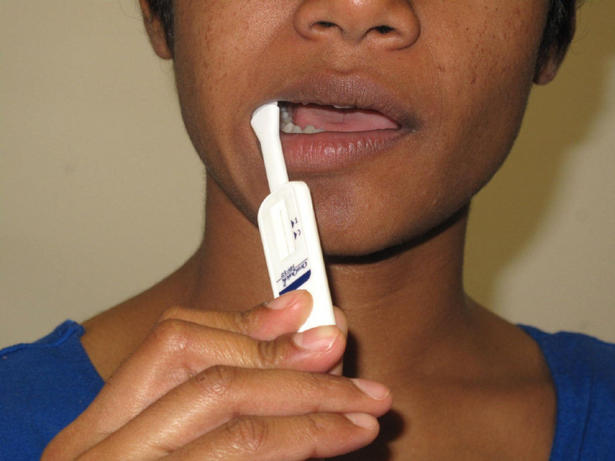
A saliva test used to diagnose the human immunodeficiency virus (HIV), is comparable in accuracy to the traditional blood test, according to a new study led by the Research Institute of the McGill University Health Centre (RI-MUHC) and McGill University. The meta-analysis, which compared studies worldwide, showed that the saliva HIV test, OraQuick HIV1/2, had the same accuracy as the blood test for high-risk populations. The test sensitivity was slightly reduced for low risk populations. The study, published in this week’s issue of The Lancet Infectious Diseases, has major implications for countries that wish to adopt self-testing strategies for HIV.
“Testing is the cornerstone of prevention, treatment and care strategies,” says the study’s lead author, Dr. Nitika Pant Pai, a medical scientist at the RI-MUHC and assistant professor of Medicine at McGill University. “Although previous studies have shown that the oral fluid-based OraQuick HIV1/2 test has great promise, ours is the first to evaluate its potential at a global level.”
Dr. Pant Pai and her colleagues analyzed and synthesized real-life field research data from five worldwide databases. Their findings showed that the saliva test is 99 percent accurate for HIV in high risk populations, and about 97 percent in low risk populations.
The oral HIV test has become one of the most popular tests because of its acceptability and ease of use. It is non-invasive, pain-free, and convenient and produces results in 20 minutes. “Getting people to show up for HIV testing at public clinics has been difficult because of visibility, stigma, lack of privacy and discrimination. A confidential testing option such as self-testing could bring an end to the stigmatization associated with HIV testing,” says Dr. Pant Pai, whose work is supported by a Grand Challenges Canada’s Rising Star in Global Health Award. “There is a huge global momentum for alternate HIV self-testing strategies that can inform people of their status.”
High risk populations fuel the expansion of HIV epidemics but they face widespread discrimination, violence and social marginalization from healthcare services. UNAIDS estimates that globally, 90% of men who have sex with men lack access to the most basic sexual health services. “Oral HIV tests can be a powerful tool for high risk populations, but self-testing must be accompanied by linkage to care to achieve good health outcomes,” says the study’s co-author Dr. Rosanna Peeling, Professor and Chair of Diagnostics Research at the London School of Hygiene & Tropical Medicine.
About this study
The study, Head-to-head comparison of accuracy of a rapid point-of-care HIV test with oral versus whole-blood specimens: a systematic review and meta-analysis, was coauthored by Nitika Pant Pai (RI-MUHC/McGill), Bhairavi Balram (McGill), Sushmita Shivkumar (McGill), Jorge M Cajas (Queen’s University, Kingston), Christiane Claessens (Institut National de santé publique du Québec), Gilles Lambert (Direction de santé publique de l’agence de la santé et des services sociaux de Montréal, INSPQ), Rosanna W Peeling (London School of Hygiene and Tropical Medicine, UK), and Lawrence Joseph (RI-MUHC/McGill).
Partners in research:
This work has been made possible by a Knowledge Syntheses Grant from Canadian Institutes of Health Research (CIHR).
Related coverage
The Lancet
CNET
Daily Mail
The Star
CTV News
The Scientist
Le Devoir (in French)
January 26, 2012
