People living with neurological diseases come to The Neuro’s Clinical Research Unit to find hope for themselves and to move science forward
Every new medication that makes it onto a prescription pad at your doctor’s office had to go through a clinical trial first to assess its safety and efficacy. Yet, there is one essential element in the clinical trial process that goes unmentioned when discussing advances in research — and that’s the patients themselves. Without their participation, progress in treating neurological diseases would come to a halt.
Partners in the process
Neurological conditions have a heavy burden of disease, and many conditions are degenerative. Individuals living with these diagnoses may have a strong motivation to help test novel treatments. “I very much believe in the work that researchers do. It contributes to our own hope as patients,” explains Ana*, who was diagnosed over 15 years ago with relapsing-remitting Multiple Sclerosis (MS), when she was 24.
Ana was prescribed medication that allowed her to remain active, practicing karate, tennis and hiking for several years, until her MS progressed. At that point, her neurologist at The Neuro (Montreal Neurological Institute-Hospital) proposed that she take part in a clinical trial testing a new medication. “I felt I had to do something. This is an illness that affects a lot of young people and taking part in a trial seemed like a good way to help further science.”
Thanks to patients, the treatment landscape has changed considerably in the past decade. “There are more approved treatments for neurological diseases than ever before,” asserts Angela Genge, MD, the executive director of the Clinical Research Unit at The Neuro (CRU), one of the largest neurological research centres in Canada, conducting over 115 clinical trials each year. “We are studying investigational treatments that would be the first approved therapies for a number of rare diseases. And we are also studying ways to lessen the burden of disease for patients, for example with new oral formulations for therapies that were previously given by IV infusion.”
 At the heart of clinical research
At the heart of clinical research
Patients are essential partners at the CRU. “We are grateful for people choosing to give their time to help advance research. We really couldn’t do what we do without them,” believes Dr. Genge. “They are incredible people. Many will participate in clinical trials despite having limited time left and knowing that they won’t see the benefit themselves.”
A lack of new treatment options and the hope of contributing to a breakthrough therapy prompted Kevin*, who was diagnosed with Parkinson’s Disease (PD) at 60, to take part in a trial. “There hasn’t been a new drug to treat Parkinson’s in decades. But technology keeps advancing. Researchers are going to come up with something that can stop the progression of the disease, like they have for cancer,” he states. The owner of a financial services firm and an avid sportsman who competed in triathlons, Kevin doesn’t want to let PD slow him down. “If a new treatment works, and you’re in that clinical trial, you have access to that treatment right away. That is definitely a plus. If not, you might have to wait years,” he says.
Working with Open Science
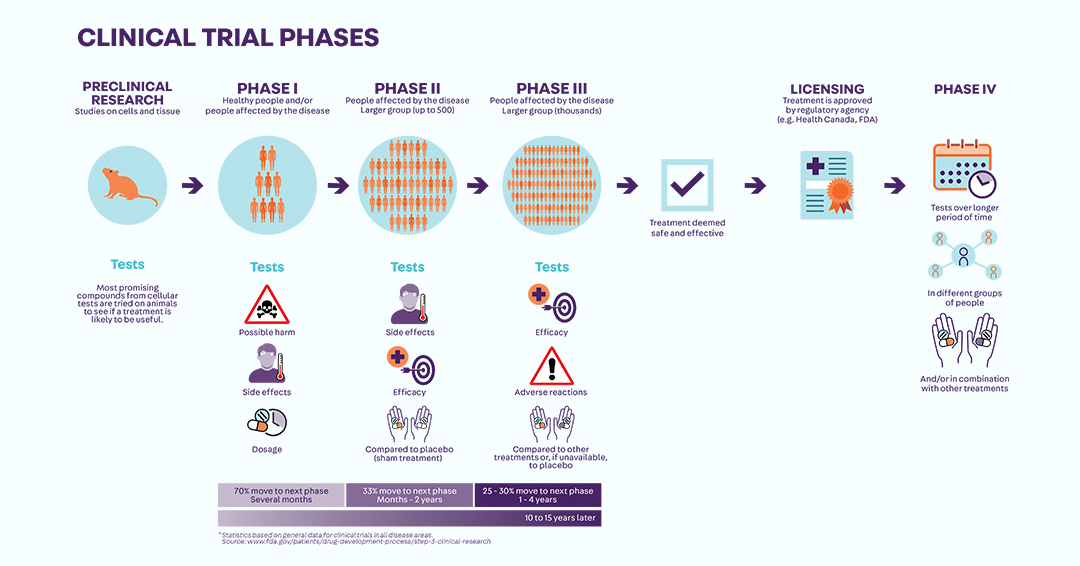
Clinical trials are just the last in a long series of steps needed for a new treatment to be approved. Before any treatments can be developed, extensive research is needed into mechanisms underlying the progression of the disease. Patients can contribute to this crucial early stage by taking part in observational studies and biobanking initiatives, where no drug is being tested.
Initiatives at the CRU such as CAPTURE ALS and DEMySTIFI (Data Extraction in Multiple Sclerosis To Inform Future Interventions) capture patient biosamples and clinical data. These types of initiatives allow researchers around the world to test new hypotheses with a much larger pool of patients – which is key, particularly for rare disease. These initiatives contribute to the anonymized biosamples and patient data collected in The Neuro’s C-BIG Repository, one of the largest biorepositories for neurological disorders in the world.
From start to finish, developing and conducting all the phases of a clinical trial takes years. While not all trials will yield an approved treatment, all research helps advance our understanding of a disease and its possible treatment pathways, if only by ruling out certain avenues of study and reorienting research.
For Ana, whenever her neurologist proposes a new trial, she is ready to participate. “Without research we are left with the status quo, and for me the status quo is not an option,” she insists.
For more about clinical trials at the CRU, visit cru.mcgill.ca.
For more on the participating in clinical trials in Canada, consult Health Canada and the It Starts With Me.
*To protect the privacy of patients, pseudonyms have been used.
