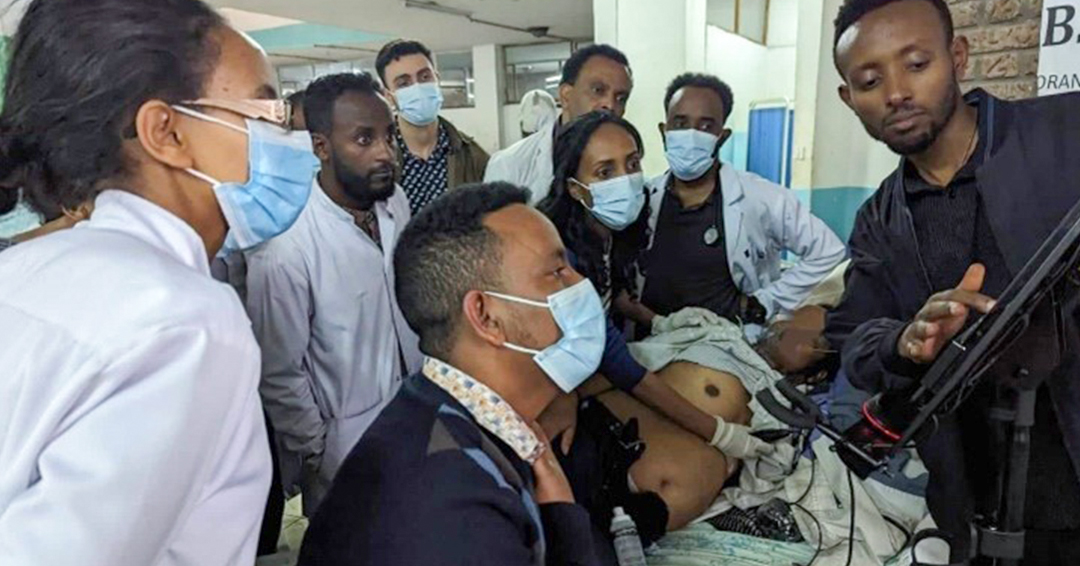
Step into Ethiopia’s healthcare system, where Drs Jonathan Houle, Ning-Zi Sun, Louise Pilote, and two McGill alumni, Drs Mark Clarfield and Ora Paltiel, of the McGill Department of Medicine, spearheaded a project titled “Enhancing Clinical and Critical Appraisal Skills in a Provincial Medical School in Ethiopia.” Generously funded by the Royal College of Physicians and Surgeons of Canada’s International Development and Aid Grant, this project aimed to enhance medical education in the region through training the physicians of a local medical school and hospital. Dr. Houle kindly shared a summary of their recent trip to Ethiopia below.
 “A portion of our project consists of developing and implementing a setting-adapted point-of-care ultrasound (POCUS) curriculum for the needs of the University of Gondar Hospital (UGH) in the Amhara region in Northern Ethiopia. A full POCUS curriculum was completed in Montreal over the last two years. Both the development and delivery of the curriculum were greatly delayed by the pandemic and by local conflict in the Tigray and neighboring provinces of Ethiopia which precluded traveling to the Amhara region. Though a peace treaty was signed in November 2022 in Ethiopia, because of many other subsequent conflicts in Northern Ethiopia, to this day the government of Canada still recommends avoiding travel to the Amhara region and therefore McGill University forbids visiting Gondar reasons related to its academic mission. It was decided that the training would take place in the capital, Addis Ababa, where the level of risk has remained low over the last two years of the conflict and where McGill allows us to travel. Physicians from UGH were flown into Addis Ababa for the training.
“A portion of our project consists of developing and implementing a setting-adapted point-of-care ultrasound (POCUS) curriculum for the needs of the University of Gondar Hospital (UGH) in the Amhara region in Northern Ethiopia. A full POCUS curriculum was completed in Montreal over the last two years. Both the development and delivery of the curriculum were greatly delayed by the pandemic and by local conflict in the Tigray and neighboring provinces of Ethiopia which precluded traveling to the Amhara region. Though a peace treaty was signed in November 2022 in Ethiopia, because of many other subsequent conflicts in Northern Ethiopia, to this day the government of Canada still recommends avoiding travel to the Amhara region and therefore McGill University forbids visiting Gondar reasons related to its academic mission. It was decided that the training would take place in the capital, Addis Ababa, where the level of risk has remained low over the last two years of the conflict and where McGill allows us to travel. Physicians from UGH were flown into Addis Ababa for the training.
 The purpose of this trip was to consolidate our relationship with UGH and its physicians, as well as to “train the trainers,” i.e. to train those physicians who work at UGH and who will assume a supervisory and teaching role in the POCUS curriculum afterwards. This was done successfully during this trip as will be detailed here.
The purpose of this trip was to consolidate our relationship with UGH and its physicians, as well as to “train the trainers,” i.e. to train those physicians who work at UGH and who will assume a supervisory and teaching role in the POCUS curriculum afterwards. This was done successfully during this trip as will be detailed here.
A medical student named Omar Idrissi and I landed in Addis Ababa on July 17, 2023. Omar was recruited as part of a global health program at McGill where students compete to join ongoing global health initiatives for the summer. For the most part, Omar’s trip was paid by this program. Omar is a keen young physician with POCUS expertise and was a great help with the preparation of the trip and took on some of the lectures we gave during the training.
 The training took place in a satellite hospital of St-Paul’s Hospital, called AaBET Hospital, which is also a public hospital in Addis Ababa. There, we had access to a room to teach for a week. In exchange, our contacts at St-Paul’s hospital asked if we would be willing to teach a few of their residents and physicians, which we accepted. The full training was three days from 9h00 AM to 5h00 PM. We separated the learners from Gondar into two groups of three physicians from to avoid service interruption at UGH and to optimize the learning experience. Physicians and residents from St. Paul Hospital were also invited to join. Most of those who attended came for half days here and there, as they still had to attend to their clinical duties, but some of them attended most of the training. In total we offered training to approximately ten physicians. However, we only evaluated the learners from UGH (6 physicians).
The training took place in a satellite hospital of St-Paul’s Hospital, called AaBET Hospital, which is also a public hospital in Addis Ababa. There, we had access to a room to teach for a week. In exchange, our contacts at St-Paul’s hospital asked if we would be willing to teach a few of their residents and physicians, which we accepted. The full training was three days from 9h00 AM to 5h00 PM. We separated the learners from Gondar into two groups of three physicians from to avoid service interruption at UGH and to optimize the learning experience. Physicians and residents from St. Paul Hospital were also invited to join. Most of those who attended came for half days here and there, as they still had to attend to their clinical duties, but some of them attended most of the training. In total we offered training to approximately ten physicians. However, we only evaluated the learners from UGH (6 physicians).
Most learners already had some informal POCUS training and were already familiar with the settings of the ultrasound machine and basic technique and scans. However, none of them had previously received formal POCUS training and much had to be taught. Our curriculum was both intensive and extensive.
 We covered the following topics: knobology and physics of ultrasound, abdominal free fluid, subxiphoid cardiac view, abdominal aortic aneurysm, pneumothorax, hemothorax/pleural effusion, extended fast assessment with sonography in trauma (eFAST), advanced cardiac views (parasternal and apical views), inferior vena cava, rapid ultrasound for shock and hypotension (RUSH) and DVT. With more advanced trainees we also taught valve evaluations in 2D, M-mode and even spectral doppler, though the device we are donating does not have spectral doppler capacity. Each session was followed by ample time to practice. I had brought my own butterfly IQ+ device and therefore we could have two simultaneous scanning teams.
We covered the following topics: knobology and physics of ultrasound, abdominal free fluid, subxiphoid cardiac view, abdominal aortic aneurysm, pneumothorax, hemothorax/pleural effusion, extended fast assessment with sonography in trauma (eFAST), advanced cardiac views (parasternal and apical views), inferior vena cava, rapid ultrasound for shock and hypotension (RUSH) and DVT. With more advanced trainees we also taught valve evaluations in 2D, M-mode and even spectral doppler, though the device we are donating does not have spectral doppler capacity. Each session was followed by ample time to practice. I had brought my own butterfly IQ+ device and therefore we could have two simultaneous scanning teams.
An important part of this project will be the evaluation of learners and rigorous POCUS-related data collection. As such we designed a tailored POCUS station constructed around the Butterfly IQ+™ device that makes having multiple users easier while also facilitating data collection. This design also retains most of the portability of the device which can still easily be transported from one unit to another or from a floor to another using stairs (elevators are often broken and transporting traditional ultrasound machines from floor to floor was very challenging). The device’s design is based on a comprehensive needs assessment previously conducted: The station has two uninterrupted power supply devices to protect the tablet and probe but also to provide over 12h (24-72h of clinical work) of continuous scanning in the event of a prolonged power failure. All parts are easily obtained online and can be quickly delivered to Ethiopia. They do not require any special expertise to service or repair. As part of the training, we in fact covered with volunteers an additional session to teach them how to safely take apart the station, put it back together and replace sensitive parts if needed.
This trip was a complete success. We consolidated our relationship with UGH’s physicians, discussed and clarified the objectives of the project, ensure buy-in from local stakeholders and provided the necessary training for local faculty to supervise the curriculum’s delivery. The next steps are to obtain ethics approval at UGH and to deliver the curriculum to the learners.”
- Dr. Jonathan Houle MDCM, FRCPC

